Randomized controlled trials comparing dietary patterns show that vegetarian/vegan, Mediterranean, and low-carbohydrate diets improve multiple cardiovascular and metabolic outcomes, though with different effect profiles. The evidence demonstrates modest but consistent benefits for weight loss, blood pressure, and lipid parameters across most dietary patterns, with effects generally diminishing after 6–12 months.
Vegetarian and Vegan Diets
Lipid effects: Meta-analysis of 30 RCTs found vegetarian and vegan diets reduced total cholesterol by -0.34 mmol/L, LDL cholesterol by -0.30 mmol/L, and apolipoprotein B by -12.92 mg/dL compared to omnivorous diets, with consistent effects across age, health status, and study duration [1]. HDL cholesterol was also reduced by -0.082 mmol/L [2]. No significant effect on triglycerides was observed [1].
Metabolic outcomes: In patients with type 2 diabetes, vegan diets improved HbA1c levels, weight, total and LDL cholesterol, and quality of life compared to standard diabetic guidelines [3]. An umbrella review of meta-analyses found vegetarian diets reduced blood glucose and improved insulin sensitivity [2].
Blood pressure: Systematic review of 11 RCTs showed no overall blood pressure difference, but in hypertensive participants at baseline, vegan diets reduced both systolic and diastolic blood pressure [3].
Limitations: Vegetarian diets are associated with lower vitamin B12 concentrations and higher homocysteine levels, indicating adverse effects on one-carbon metabolism [2]. No RCT data exist for cardiovascular event rates, cognitive impairment, or cancer outcomes—only observational data support these associations [4].
Low-Carbohydrate Diets
Weight and body composition: Cochrane review of 61 RCTs (6,925 participants) found low-carbohydrate diets produced modest additional weight loss of -1.07 kg at 3–8.5 months and -0.93 kg at 1–2 years compared to balanced-carbohydrate diets in participants without diabetes [5]. In those with type 2 diabetes, differences were -1.26 kg at 3–6 months and -0.33 kg at 1–2 years [5]. Recent meta-analysis of 174 RCTs showed significant reductions in all body composition markers [6].
Lipid profile: Low-carbohydrate diets significantly reduced triglycerides by -15.11 mg/dL and increased HDL cholesterol by 2.92 mg/dL, but modestly increased LDL cholesterol by 4.81 mg/dL and total cholesterol by 4.32 mg/dL [6]. Ketogenic diets produced greater LDL and total cholesterol increases than moderate-carbohydrate approaches [6]. Meta-analysis of 12 RCTs confirmed triglyceride reduction of -0.15 mmol/L [7].
Blood pressure: Low-carbohydrate diets reduced systolic blood pressure by -2.05 mmHg and diastolic by -1.26 mmHg [6]. Another meta-analysis found reductions of -1.41 mmHg systolic and -1.71 mmHg diastolic [7].
Glycemic control: Meta-analysis of 149 RCTs demonstrated significant improvements in fasting glucose (-2.94 mg/dL), insulin (-8.19 pmol/L), and HOMA-IR (-0.54), with benefits most pronounced in individuals with type 2 diabetes, obesity, and females [8]. Effects were similar in isocaloric versus non-isocaloric comparisons, suggesting macronutrient composition contributes independently [8].
Inflammatory markers: Low-carbohydrate diets reduced C-reactive protein and TNF-α [6].
Diet type differences: Moderate-carbohydrate diets offered balanced benefits, while ketogenic diets produced greater weight loss but greater LDL increases. Combined fat and protein replacements yielded the most comprehensive improvements [6,8].
Comparative Effectiveness Across Dietary Patterns
Mediterranean diet: Demonstrated the strongest and most consistent evidence across outcomes. Compared to minimal intervention, Mediterranean diets reduced all-cause mortality (OR 0.72), cardiovascular mortality (OR 0.55), stroke (OR 0.65), and non-fatal MI (OR 0.48) based on moderate certainty evidence from 12 trials [9]. An umbrella review rated Mediterranean diet evidence as having the strongest validity for improving anthropometric parameters and cardiometabolic risk factors [10]. Benefits persisted at 12 months, unlike most other dietary patterns [11].
Low-fat diets: Reduced all-cause mortality (OR 0.84) and non-fatal MI (OR 0.77) with moderate certainty evidence from 18 trials [9]. At 6 months, low-fat diets produced weight loss of 4.37 kg and blood pressure reductions similar to low-carbohydrate diets [11].
DASH diet: Showed weight loss of 3.6 kg and blood pressure reductions of 4.7/2.9 mmHg at 6 months [11]. Most effective for systolic blood pressure reduction (MD -7.81 mmHg) in network meta-analysis [12].
Comparative weight loss at 6 months: Low-carbohydrate and low-fat diets had similar effects (4.63 vs 4.37 kg) [11]. Among named diets, Atkins showed largest weight reduction (5.5 kg), followed by Zone (4.1 kg) and DASH (3.6 kg) [11]. However, weight loss diminished substantially at 12 months across all dietary patterns except Mediterranean [11].
Lipid effects comparison: Low-carbohydrate diets had less LDL reduction than low-fat (1.01 vs 7.08 mg/dL) but greater HDL increase (2.31 vs -1.88 mg/dL) [11]. Network meta-analysis found low-carbohydrate and low-fat diets most effective for HDL increase [12].
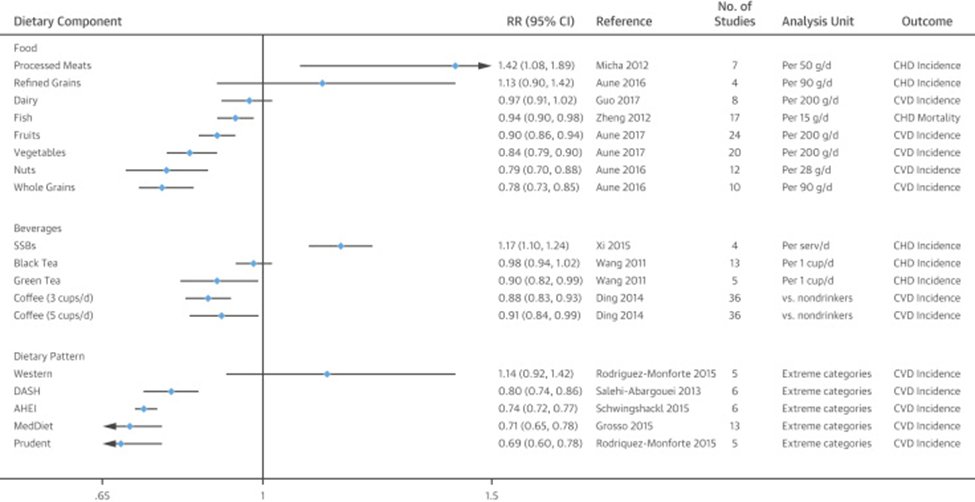
Summary of Various Meta-Analyses for the Associations of Key Foods and Food Groups, and Dietary Patterns With Incident CVD (Reprint Of Figure 2 from Reference [13])
Duration of Effects
A critical finding across multiple meta-analyses is that benefits for weight reduction and cardiovascular risk factors largely disappear at 12 months for most dietary interventions, with the notable exception of the Mediterranean diet, which maintains benefits [9,11]. This highlights challenges with long-term dietary adherence and sustainability.
Evidence Quality
Most systematic reviews rated evidence quality as moderate to low using GRADE methodology [5,10]. Common limitations included high risk of bias from missing outcome data, heterogeneity in diet definitions, and lack of long-term follow-up. Importantly, no RCT data exist for hard cardiovascular endpoints (MI, stroke, cardiovascular death) for vegetarian/vegan diets—only observational data support these associations [4].
References
[1]. Vegetarian or Vegan Diets and Blood Lipids: A Meta-Analysis of Randomized Trials. Koch CA, Kjeldsen EW, Frikke-Schmidt R. European Heart Journal. 2023;44(28):2609-2622. doi:10.1093/eurheartj/ehad211.
[2]. Health Outcomes Associated With Vegetarian Diets: An Umbrella Review of Systematic Reviews and Meta-Analyses. Oussalah A, Levy J, Berthezène C, Alpers DH, Guéant JL. Clinical Nutrition (Edinburgh, Scotland). 2020;39(11):3283-3307. doi:10.1016/j.clnu.2020.02.037.
[3]. Vegan Dietary Pattern for the Primary and Secondary Prevention of Cardiovascular Diseases. Rees K, Al-Khudairy L, Takeda A, Stranges S. The Cochrane Database of Systematic Reviews. 2021;2:CD013501. doi:10.1002/14651858.CD013501.pub2.
[4]. Vegetarian and Vegan Diets: Benefits and Drawbacks. Wang T, Masedunskas A, Willett WC, Fontana L. European Heart Journal. 2023;44(36):3423-3439. doi:10.1093/eurheartj/ehad436.
[5]. Low-Carbohydrate Versus Balanced-Carbohydrate Diets for Reducing Weight and Cardiovascular Risk. Naude CE, Brand A, Schoonees A, et al. The Cochrane Database of Systematic Reviews. 2022;1:CD013334. doi:10.1002/14651858.CD013334.pub2.
[6]. Effects of Carbohydrate-Restricted Diets and Macronutrient Replacements on Cardiovascular Health and Body Composition in Adults: A Meta-Analysis of Randomized Trials. Feng S, Liu R, Thompson C, et al. The American Journal of Clinical Nutrition. 2025;:S0002-9165(25)00528-3. doi:10.1016/j.ajcnut.2025.09.012.
[7]. The Effects of Low-Carbohydrate Diets on Cardiovascular Risk Factors: A Meta-Analysis. Dong T, Guo M, Zhang P, Sun G, Chen B. PloS One. 2020;15(1):e0225348. doi:10.1371/journal.pone.0225348.
[8]. Carbohydrate-Restricted Diet Types and Macronutrient Replacements for Metabolic Health in Adults: A Meta-Analysis of Randomized Trials. Feng S, Liu R, Colwell B, et al. Clinical Nutrition (Edinburgh, Scotland). 2025;54:27-41. doi:10.1016/j.clnu.2025.09.005.
[9]. Comparison of Seven Popular Structured Dietary Programmes and Risk of Mortality and Major Cardiovascular Events in Patients at Increased Cardiovascular Risk: Systematic Review and Network Meta-Analysis. Karam G, Agarwal A, Sadeghirad B, et al. BMJ (Clinical Research Ed.). 2023;380:e072003. doi:10.1136/bmj-2022-072003.
[10]. Effects of Popular Diets on Anthropometric and Cardiometabolic Parameters: An Umbrella Review of Meta-Analyses of Randomized Controlled Trials. Dinu M, Pagliai G, Angelino D, et al. Advances in Nutrition (Bethesda, Md.). 2020;11(4):815-833. doi:10.1093/advances/nmaa006.
[11]. Comparison of Dietary Macronutrient Patterns of 14 Popular Named Dietary Programmes for Weight and Cardiovascular Risk Factor Reduction in Adults: Systematic Review and Network Meta-Analysis of Randomised Trials. Ge L, Sadeghirad B, Ball GDC, et al. BMJ (Clinical Research Ed.). 2020;369:m696. doi:10.1136/bmj.m696.
[12]. Comparative Effect of Dietary Patterns on Selected Cardiovascular Risk Factors: A Network Study. Sun Y, Shang M, Zhang Y, Hu J, Wang H. Scientific Reports. 2025;15(1):28749. doi:10.1038/s41598-025-13596-x.
[13]. Reprint Of: Cardiovascular Disease Prevention by Diet Modification: JACC Health Promotion Series. Yu E, Malik VS, Hu FB. Journal of the American College of Cardiology. 2018;72(23 Pt B):2951-2963. doi:10.1016/j.jacc.2018.10.019.

